
Contractor Charged for Defrauding Liberty Mutual of $9 Million in Insurance Premiums
Georgia contractor Jose Martinez faces charges for defrauding Liberty Mutual Insurance by underreporting payroll, impacting workers’ compensation premiums.
January 4, 2024
Fraud
Insurance Industry
Legislation & Regulation
Workers' Compensation
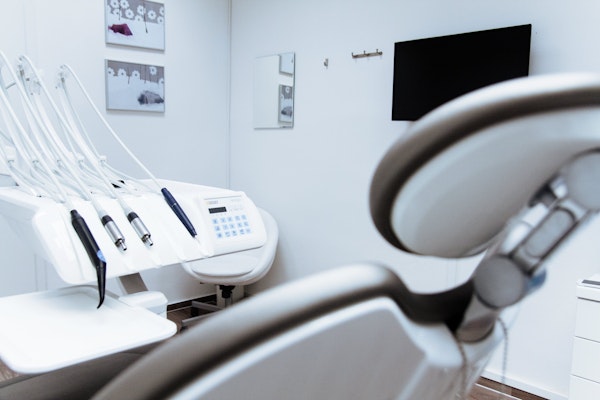
Minnesota Woman Sues Dentist Over Extensive, Allegedly Harmful Dental Procedures
A Minnesota woman sues her dentist for alleged negligence, claiming extensive dental work in one visit led to disfigurement and health issues.
January 3, 2024
Liability
Life & Health
Litigation
Risk Management
Minnesota
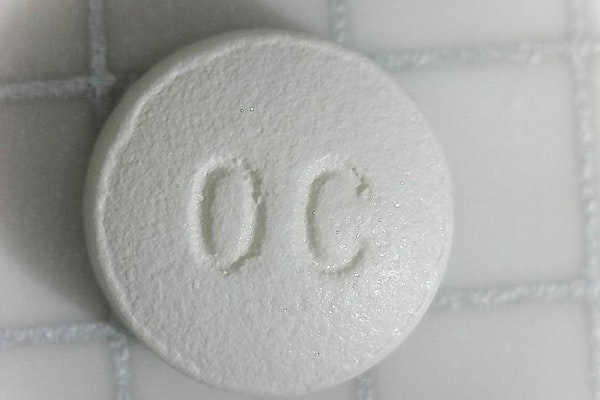
McKinsey Agrees to $78 Million Settlement in Prescription Opioid Crisis
McKinsey and Company will establish a $78 million fund to reimburse insurers and others for costs related to the prescription opioid addiction crisis.
January 3, 2024
Insurance Industry
Life & Health
Risk Management

Court Upholds New York Fund’s Authority to Surcharge Noncash Tips for Black Car Drivers
A Second Circuit Court ruling supports the New York workers’ compensation fund’s authority to impose a surcharge on noncash tips for black car drivers.
January 3, 2024
Auto
Insurance Industry
Legislation & Regulation
Workers' Compensation
New York

January 1 Renewals Mark a Turnaround in Reinsurance Market Stability
The January 1 reinsurance renewal period exhibits stability and predictability, reflecting significant improvements in the property reinsurance sector.
January 3, 2024
Catastrophe
Insurance Industry
Property
Risk Management

Revolutionizing Auto Insurance in the Era of New Vehicle Valuation Trends
Exploring the shift in vehicle valuation methods in auto insurance, highlighting the rise of SUVs and the impact of consumer preferences on risk management.
January 3, 2024
Auto
Insurance Industry
Risk Management
Technology
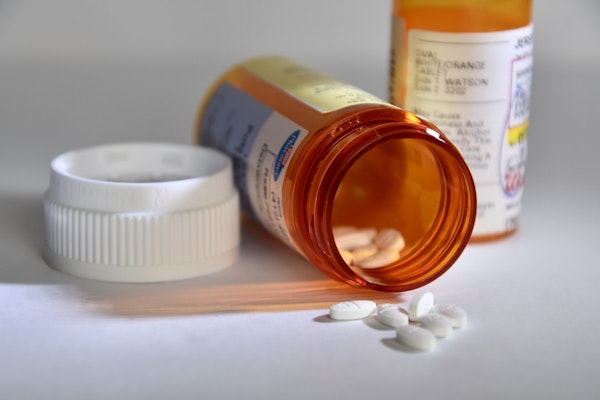
The Evolving Dynamics of Pharmacy Use in Workers’ Compensation
Exploring the top five pharmacy trends in workers’ compensation for 2024, focusing on physician dispensing, mental health, opioids, long COVID, and inflation.
January 3, 2024
Legislation & Regulation
Life & Health
Risk Management
Workers' Compensation
Florida

Navigating the New Frontier in Cannabis Insurance and Legal Landscape
As cannabis markets grow, insurers and legal professionals explore challenges and opportunities in a dynamically evolving industry.
January 3, 2024
Legislation & Regulation
Liability
Risk Management
Technology

Celebrating Insurance Innovation Leaders of 2023 in the Global Awards
Celebrating the achievements of AIA, PAK Insurance Programs, and Swiss Re as they lead the way in transforming the insurance industry through innovative solutions and strategies in 2023.
January 2, 2024
Catastrophe
Life & Health
Technology
Underwriting

P&C Insurance in 2023: A Year to Forget, but a Stepping Stone to Future Success
Exploring the tumultuous journey of the P&C industry in 2023 and its potential path towards recovery and innovation in 2024, amidst global and economic uncertainties.
January 2, 2024
Auto
Catastrophe
Legislation & Regulation
Technology
Alabama
California
Florida
Louisiana
Mississippi

Navigating Unpredictable Futures: Key Predictions for Insurance in 2024 and Beyond
Exploring the evolving landscape of insurance in 2024, with a focus on technology, industry consolidation, and the impact of climate change on insurance strategies.
January 2, 2024
Auto
Catastrophe
Legislation & Regulation
Technology

Allianz Report: Rising Liability Risks for Directors and Officers in 2024
Allianz Commercial’s latest report highlights heightened liability risks for board members and executives in 2024, including economic, geopolitical, technological, and ESG challenges.
January 2, 2024
Legislation & Regulation
Liability
Risk Management
Technology

Aon’s Survey Reveals Increasing Business Volatility and Emerging Global Risks
Aon’s ninth edition of its Global Risk Management Survey highlights a more volatile and uncertain business landscape, with cybersecurity and economic challenges at the forefront.
December 29, 2023
Catastrophe
Insurance Industry
Risk Management
Technology

BlendJet Recalls Millions of Portable Blenders Due to Safety Hazards
BlendJet issues a recall for 4.8 million portable blenders after reports of lacerations, burn injuries, and fire hazards, urging consumers to seek replacements.
December 29, 2023
Liability
Risk Management

Chesapeake Energy and Contractors Faulted in Fatal 2020 Texas Oil Well Fire
A federal safety board investigation finds Chesapeake Energy and its contractors failed to implement crucial well control measures in a 2020 Texas oil well fire that resulted in three fatalities.
December 29, 2023
Catastrophe
Legislation & Regulation
Liability
Risk Management
Oklahoma
Texas





